The Link Between Gum Disease and Heart Disease, Diabetes, and Alzheimer’s
Is Gum Disease Connected to Other Health Problems?
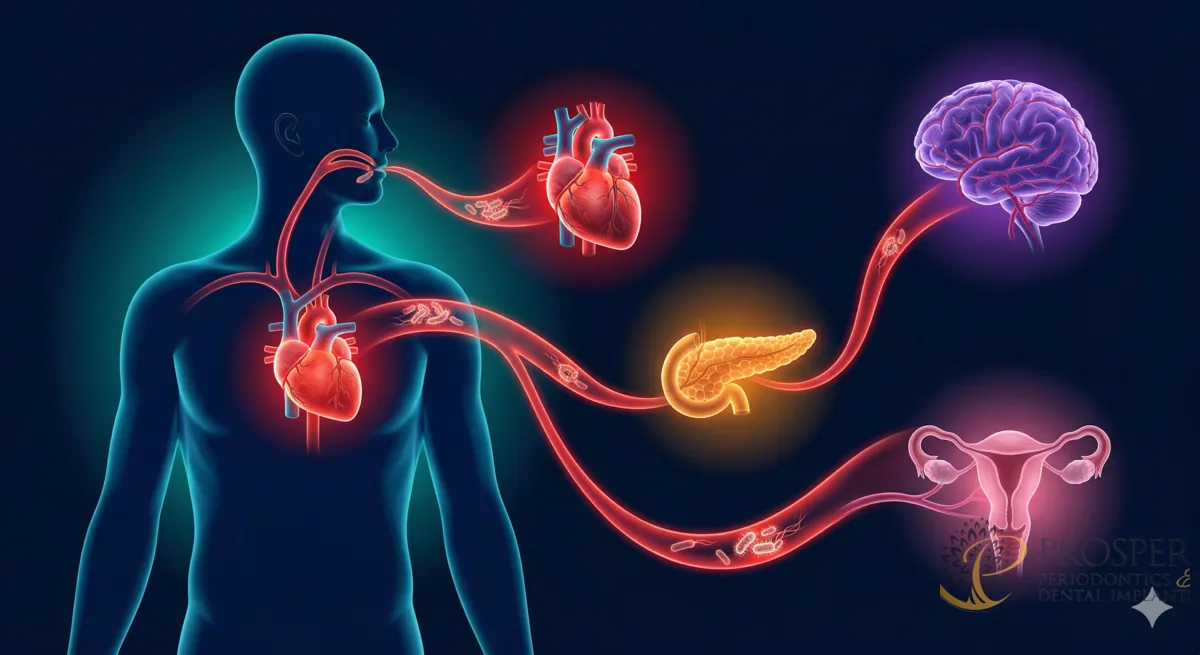
Yes — decades of medical research have established strong links between periodontal disease and several serious systemic conditions, including heart disease, diabetes, Alzheimer’s disease, and pregnancy complications. The bacteria that cause gum disease can enter the bloodstream and trigger inflammation throughout the body.
Gum Disease and Heart Disease
People with periodontitis are 2 to 3 times more likely to have a heart attack, stroke, or other cardiovascular event. The oral bacteria Porphyromonas gingivalis has been found in arterial plaque — the deposits that cause heart attacks. Research published by the American Heart Association has confirmed that periodontal disease is an independent risk factor for cardiovascular disease.
Gum Disease and Diabetes
The relationship between gum disease and diabetes is bidirectional — each condition makes the other worse. Uncontrolled diabetes increases susceptibility to gum infections, while active periodontitis makes blood sugar harder to control. Treating gum disease has been shown to improve HbA1c levels in diabetic patients, according to research in the Journal of Clinical Periodontology.
Gum Disease and Alzheimer’s Disease
The same bacteria that cause gum disease (P. gingivalis) have been found in the brains of Alzheimer’s patients. A landmark study published in Science Advances (2019) identified gingipains — toxic enzymes produced by P. gingivalis — in the brain tissue of Alzheimer’s patients, suggesting a direct pathological link.
Gum Disease and Pregnancy Complications
Pregnant women with untreated periodontitis have a higher risk of preterm birth and low birth weight. The inflammatory response triggered by gum disease can affect the developing fetus. The American Academy of Periodontology recommends that pregnant women receive periodontal evaluation and treatment during pregnancy.
How Treating Gum Disease Protects Your Whole Body
By eliminating the chronic bacterial infection in your gums, you reduce the inflammatory burden on your entire body. Treatments like LANAP laser therapy and professional periodontal care do more than save your teeth — they contribute to your overall health and longevity.
“I always tell my patients that their mouth is the gateway to their body,” says Dr. Parachuru. “Treating gum disease is not just about saving teeth — it is about protecting your heart, your brain, and your quality of life.”
Schedule your periodontal evaluation today. Call (972) 787-1122 or book online.
How Does Gum Disease Actually Trigger Inflammation in the Rest of the Body?
The mouth is not an isolated system. When bacteria colonize below the gumline, they release toxins that damage the connective tissue and bone supporting your teeth. But the damage does not stop there. Those same bacteria, along with the inflammatory proteins your immune system produces in response, can travel through the thin walls of the gum tissue directly into the bloodstream. From there, they circulate to the heart, brain, lungs, kidneys, and joints.
The primary mechanism is systemic inflammation driven by cytokines. Specifically, your immune system releases interleukin-1-beta (IL-1-beta), tumor necrosis factor-alpha (TNF-alpha), and C-reactive protein (CRP) in response to periodontal infection. These same inflammatory markers are found at elevated levels in patients with cardiovascular disease, type 2 diabetes, and Alzheimer’s disease. This shared inflammatory pathway is why researchers now view the mouth as a window into whole-body health.
Patients with advanced periodontitis show CRP levels significantly above those of healthy individuals. CRP is one of the most reliable predictors of heart attack risk used in cardiology today. Treating the gum infection has been shown in multiple studies to reduce CRP levels within 3 to 6 months of successful periodontal therapy.
Clinical Evidence
Successful periodontal treatment significantly reduces systemic levels of C-reactive protein and interleukin-6, inflammatory markers linked to cardiovascular disease risk. — Journal of Periodontology (D'Aiuto et al., 2004)
What Is the Specific Mechanism Connecting Gum Disease and Heart Disease?
The connection between periodontal disease and cardiovascular disease is more direct than most patients realize. The bacterium Porphyromonas gingivalis does not simply inflame the gums. When it enters the bloodstream, it has the ability to invade the endothelial cells that line blood vessel walls. Once inside, it triggers platelet aggregation – the same process that forms dangerous clots in coronary arteries.
In autopsy studies, P. gingivalis DNA has been identified in atherosclerotic plaques of patients who died from heart attacks. The same bacteria causing the infection in your gums can be found clogging the arteries feeding your heart. This is not a statistical correlation – it is a direct biological pathway. A large-scale review by the American Heart Association concluded that periodontal disease is an independent risk factor for cardiovascular disease, meaning the risk exists even after accounting for shared factors like smoking, diet, and age.
The risk is quantified and it is significant. People with severe periodontitis are approximately 2 to 3 times more likely to experience a fatal heart attack compared to those with healthy gums. For stroke, the relative risk increases by roughly 2 times. These numbers come from population studies involving tens of thousands of patients followed over decades.
Expert Insight
“What concerns me most is that many of my patients with advanced gum disease have no idea their cardiovascular risk is elevated. When I see deep pockets, bone loss, and active bleeding, I am looking at chronic systemic inflammation - not just a dental problem. Treating the periodontal infection is one of the most evidence-based interventions we have for lowering that inflammatory burden and protecting heart health.”
— Dr. Parachuru, Periodontist
How Does Treating Gum Disease Improve Blood Sugar Control in Diabetic Patients?
The relationship between periodontal disease and diabetes is one of the best-documented bidirectional relationships in all of medicine. Uncontrolled blood sugar creates an environment where periodontal bacteria thrive. High glucose levels impair white blood cell function, reduce the body’s ability to fight infection, and slow tissue healing – all of which allow gum disease to advance faster and more severely in diabetic patients.
In the other direction, active periodontal infection directly worsens insulin resistance. The inflammatory cytokines released by gum disease – particularly TNF-alpha – interfere with insulin receptor signaling, making it harder for cells to absorb glucose from the blood. This creates a feedback loop: diabetes makes gum disease worse, and gum disease makes blood sugar harder to control.
The clinical evidence for periodontal treatment improving HbA1c is compelling. Multiple randomized controlled trials have demonstrated that patients with type 2 diabetes who received thorough periodontal treatment – including scaling and root planing or laser therapy – showed meaningful reductions in HbA1c levels of 0.3 to 0.5 percentage points at 3 to 6 months post-treatment. While that may sound small, it is clinically equivalent to adding a second oral diabetes medication for some patients.
Clinical Evidence
Periodontal treatment in patients with type 2 diabetes resulted in statistically significant reductions in HbA1c at 3 to 4 months post-treatment, supporting the bidirectional relationship between periodontal and metabolic disease. — Journal of Clinical Periodontology (Simpson et al., 2015)
For patients managing diabetes in the Prosper and Frisco area, this means your periodontal health is a legitimate component of your diabetes management plan. A periodontist and your primary care physician or endocrinologist should be communicating. At Prosper Periodontics, Dr. Parachuru routinely collaborates with patients’ medical teams when systemic health connections are present. Learn more about comprehensive periodontal care and how it fits into your overall health picture.
What Does the Research Say About Gum Disease and Alzheimer’s Risk?
The Alzheimer’s connection is the newest and perhaps most alarming chapter in this research. For years, researchers suspected a link because Alzheimer’s patients tend to have poor oral hygiene and more severe gum disease. But the question was whether gum disease was a cause or simply a byproduct of cognitive decline making self-care difficult.
A landmark 2019 study published in Science Advances shifted that debate significantly. Researchers from Cortexyme identified gingipains – toxic proteases produced specifically by Porphyromonas gingivalis – in the brain tissue of 96 percent of Alzheimer’s cases examined at autopsy. The same bacteria were found alive in the spinal fluid of living Alzheimer’s patients. In animal models, oral infection with P. gingivalis led to brain colonization by the bacteria, subsequent production of amyloid beta (the protein associated with Alzheimer’s plaques), and neurodegeneration – a causal chain, not just an association.
Longitudinal population data adds to this picture. A study following 9,291 participants over 18 years found that people with chronic periodontitis had a 70 percent increased risk of developing Alzheimer’s disease compared to those without gum disease. Researchers adjusted for age, sex, education, smoking, and cardiovascular history – the gum disease risk remained independent of all of these factors.
The brain’s vulnerability stems from two pathways. First, oral bacteria can travel to the brain via the trigeminal nerve, which connects the teeth and jaws directly to brainstem structures. Second, the systemic inflammatory response driven by gum disease promotes neuroinflammation, which accelerates the accumulation of beta-amyloid plaques and tau protein tangles associated with Alzheimer’s pathology.
Is There Evidence That Periodontal Treatment Can Reduce These Systemic Risks?
This is the question patients ask most often – and the short answer is yes, with important caveats. Multiple clinical trials have demonstrated that successful periodontal treatment reduces the systemic inflammatory burden. CRP levels drop. TNF-alpha levels fall. Endothelial function – a measure of blood vessel health – improves. In diabetic patients, HbA1c improves. These are measurable, biologically meaningful changes.
The key word is “successful.” A single cleaning is not sufficient to reverse chronic periodontitis. Treatment must achieve bacterial reduction below the gumline, elimination of the infected pocket tissue, and long-term suppression of the pathogenic bacterial load through periodontal maintenance. This is why the standard of care for treated periodontitis patients is a professional cleaning every 3 to 4 months – not the standard 6-month interval recommended for healthy patients.
Advanced treatment options like LANAP laser therapy are particularly effective at achieving the bacterial decontamination required to reduce systemic inflammation. The 1064nm wavelength of the PerioLase MVP-7 laser selectively destroys gram-negative anaerobic bacteria – the specific class responsible for systemic complications – while leaving healthy tissue intact. Patients who undergo LANAP treatment and maintain regular periodontal maintenance visits show consistently improved systemic inflammatory profiles at 6- and 12-month follow-ups.
If you have been diagnosed with heart disease, diabetes, or have a family history of Alzheimer’s disease, your periodontal health deserves serious attention. A thorough periodontal evaluation at Prosper Periodontics takes less than an hour and will give you a complete picture of where you stand. The findings from that evaluation may be among the most important health information you receive this year. Read more about the warning signs of gum disease you should never ignore, and learn whether your condition is still reversible.
Who Is Most at Risk for Both Gum Disease and Systemic Complications?
Certain patient populations face compounded risk from the gum disease-systemic disease connection and deserve especially proactive periodontal monitoring. These groups include:
- Smokers and former smokers: Tobacco use is the single largest modifiable risk factor for periodontitis. Smokers are 3 to 6 times more likely to develop severe gum disease and also carry elevated cardiovascular risk from both smoking and the resulting periodontal infection.
- Patients with type 1 or type 2 diabetes: The bidirectional relationship creates a cycle that requires active management from both medical and dental providers.
- Patients with a personal or family history of heart disease: Existing cardiovascular inflammation is amplified by the chronic bacterial load from untreated periodontitis.
- Post-menopausal women: Estrogen decline accelerates bone loss, including alveolar bone. This population tends to see more rapid progression of periodontitis and should maintain more frequent periodontal monitoring.
- Patients on medications that cause dry mouth (xerostomia): Saliva is a natural defense against oral bacteria. Over 500 commonly prescribed medications reduce saliva flow, increasing susceptibility to both decay and periodontal disease.
- Patients with a history of preterm birth or pregnancy complications: Periodontal disease during pregnancy significantly elevates the risk of preterm delivery and low birth weight, and affected women have a higher baseline rate of gum disease in subsequent years.
If you fall into one or more of these categories, a baseline periodontal evaluation is not optional – it is medically prudent. Early detection and treatment of periodontitis in high-risk patients has the strongest evidence base for reducing downstream systemic complications. Schedule a periodontal evaluation at Prosper Periodontics to understand exactly where your gum health stands and what your systemic risk picture looks like.
Related Resources
Learn more about the services and topics discussed in this article:
Serving Prosper, TX and Surrounding Communities
Prosper Periodontics and Dental Implants proudly serves patients across North Dallas, including: periodontal care in Frisco, TX. Schedule your appointment today.
