Are Dental Implants Worth It? Pros, Cons, and Real Results

Are Dental Implants Worth the Investment? Let’s Look at the Numbers

Most patients ask this question honestly, and it deserves an honest answer. Dental implants cost more upfront than any other tooth replacement option. That is simply true. But cost and value are not the same thing, and when you calculate the full 25-year picture, implants typically cost less than the alternatives — not more.
Here is the comparison that changes most patients’ thinking. A traditional three-unit dental bridge replacing a single missing tooth typically costs $3,000 to $6,000 at placement. But bridges have an average lifespan of 7 to 10 years before they fail, require replacement, or damage the anchor teeth supporting them. Over 25 years, you are likely to replace that bridge two to three times, with each replacement often costing more due to additional damage to the surrounding teeth. Total cost over 25 years: $9,000 to $18,000 or more, plus the cost of managing the anchor teeth that were drilled down.
A single dental implant at Prosper Periodontics averages $3,500 to $5,500 for the complete restoration, including the implant post, abutment, and crown. With a documented success rate of 95 to 98 percent at 25 years, many patients pay that cost once and never replace the tooth again. The implant becomes a permanent fixture in your jaw, functioning identically to a natural tooth. When you divide that one-time cost across 25 years, implants are often the least expensive option on a per-year basis.
The bone loss factor adds a third cost dimension most patients never consider. When you lose a tooth and do not replace it with an implant, the jawbone beneath the empty space begins to resorb – a process that is permanent and progressive. Within one year of tooth loss, you can lose up to 25 percent of bone volume in that area. Within three years, up to 40 to 60 percent. That bone loss widens over time and can compromise adjacent teeth, alter your bite, and change the shape of your face. Reversing it requires bone grafting, which adds $500 to $3,000 to the eventual cost of any replacement. Implants eliminate this cost entirely by stimulating the bone through normal chewing forces, exactly as a natural tooth root does.
Clinical Evidence
Dental implants demonstrate survival rates of 95-98% at 10 years and maintain marginal bone levels superior to tooth-supported fixed partial dentures, making them the gold standard for single-tooth replacement. — Journal of Oral and Maxillofacial Surgery (Albrektsson et al., 2008)
What Quality-of-Life Gains Do Dental Implant Patients Actually Experience?
Clinical research on quality of life after dental implants is unusually consistent. Study after study shows significant, measurable improvements in three core domains: eating ability, speech clarity, and psychological well-being. These are not soft, subjective claims. They are scored on validated quality-of-life instruments used in peer-reviewed research.
Eating is the first place patients notice the difference. A removable denture restores about 20 to 25 percent of natural biting force. A dental bridge restores more, but patients still report avoiding hard foods like apples, corn on the cob, and raw carrots out of concern for the bridge. Dental implants restore 85 to 95 percent of natural biting force. Patients can eat the full range of foods without anxiety. In long-term follow-up studies, implant patients consistently report higher dietary satisfaction and broader food variety than denture wearers – which has measurable secondary benefits for nutrition and overall health.
Speech returns to normal immediately. Missing back teeth do not affect speech significantly, but missing front teeth alter articulation noticeably. Ill-fitting dentures are a common cause of slurred speech and clicking sounds during conversation. Because implants are fixed in the jaw and do not move, speech is identical to natural teeth from day one after the crown is placed.
The psychological impact is harder to quantify but consistently reported as life-changing by patients. Patients describe an immediate return to smiling freely in photographs, meeting people without self-consciousness, and engaging socially in ways they had avoided for months or years. Research using validated psychological instruments like the Oral Health Impact Profile (OHIP-14) shows that implant patients report higher oral-health-related quality of life than patients with any other replacement option, including bridges.
Expert Insight
“What patients tell me after implant completion is that they feel whole again. They stop avoiding foods, stop covering their mouth when they laugh, and stop canceling social plans. When a 45-year-old patient tells me they have not eaten a steak in two years because of a missing molar, and after their implant they are texting me a photo from a restaurant -- that is when you understand the real return on investment.”
— Dr. Parachuru, Periodontist
What Does the Research Say About Implant Success Rates?
Dental implant success rates are among the most extensively studied outcomes in all of dentistry. The short summary: single-tooth implant success rates in healthy patients range from 95 to 98 percent at 10 years and hold near that range at 25 years. These numbers come from decades of multicenter clinical trials and large registry studies involving hundreds of thousands of implants across multiple countries and demographic groups.
Understanding what “success” means in this context matters. Researchers define implant success as the implant remaining in the jaw, without signs of infection or bone loss beyond normal remodeling, functioning adequately, and not causing pain or discomfort. “Survival” is a slightly lower standard — the implant is still present, regardless of minor complications. The 95 to 98 percent figure reflects the stricter success criterion.
Success rates vary by placement site and patient factors. Implants placed in the lower jaw (mandible) succeed at higher rates than upper jaw (maxillary) implants due to the greater bone density of the mandible. Implants placed by specialist periodontists and oral surgeons show higher success rates than those placed by general dentists in multiple comparative studies. At Prosper Periodontics, Dr. Parachuru places all implants, which means every case is managed by a specialist with specific training in bone biology, gum tissue management, and implant protocols.
Maintenance matters significantly for long-term success. Patients who attend regular implant maintenance appointments and maintain good oral hygiene show success rates near the top of the published range. Patients who skip maintenance and develop peri-implantitis — infection around the implant — see rates closer to the lower bound. Keeping your implant clean and attending scheduled check-ups at 6-month intervals is the single most controllable factor in implant longevity.
Clinical Evidence
Systematic review of implant-supported single crowns showed 10-year survival rates of 95.2%, with higher rates for posterior mandibular implants, confirming long-term predictability of single implant restorations. — International Journal of Oral and Maxillofacial Implants (Pjetursson et al., 2007)
When Are Dental Implants NOT the Right Choice?
Intellectual honesty requires addressing this directly. Dental implants are not the right treatment for every patient, and understanding the contraindications is as important as understanding the benefits. Any provider who tells every patient they are a candidate is not being straight with you.
Uncontrolled systemic disease is the clearest contraindication. Patients with uncontrolled type 2 diabetes (HbA1c above 8.0-8.5 percent) face significantly higher implant failure rates due to impaired healing, reduced immune response, and altered bone metabolism. This does not mean diabetic patients cannot get implants — many do, successfully. It means diabetes must be well-controlled before treatment begins. Dr. Parachuru works closely with patients’ primary care physicians and endocrinologists to confirm metabolic control is adequate before proceeding.
Active smoking is the single most modifiable risk factor that reduces implant success. Smokers face failure rates two to three times higher than non-smokers. Nicotine restricts blood flow to the healing tissue, reduces the speed and completeness of osseointegration (the process by which bone fuses to the implant), and increases the risk of peri-implantitis long-term. Patients who commit to quitting smoking before implant placement and maintain cessation afterward achieve success rates approaching those of non-smokers. Patients who continue smoking throughout treatment and maintenance should have a detailed risk conversation with their periodontist before proceeding.
Severe bone loss without grafting is a temporary contraindication, not a permanent one. Many patients believe they have been told they “don’t have enough bone” for implants and assume this means implants are off the table permanently. In most cases, bone grafting can restore adequate bone volume for implant placement. The process adds 3 to 6 months to the overall timeline and increases cost, but it expands candidacy to a large proportion of patients who might otherwise be excluded.
Other situations where implants may not be the best immediate choice include: active cancer treatment involving radiation to the head and neck, certain medications that affect bone metabolism (bisphosphonates prescribed for osteoporosis require careful evaluation), active periodontal disease that has not been treated, and patients younger than 18 whose jawbones are still growing. None of these are necessarily permanent exclusions — they are reasons for a careful, timed evaluation.
What Real Patient Scenarios Show About Value
Abstract data is useful, but real patient scenarios make the decision concrete. Consider three representative cases that illustrate how the “worth it” calculation plays out differently depending on individual circumstances.
Patient A: 45-year-old with a single failing molar. The tooth has had two root canals and now needs extraction. A bridge would require grinding down the two healthy adjacent teeth, placing crowns on them, and suspending a false tooth between them. Those healthy teeth are now compromised permanently and will likely need their own crowns or root canals within 15 to 20 years. A single implant preserves both adjacent teeth, eliminates the bridge replacement cycle, and is expected to outlast the patient’s other natural teeth. The bridge is cheaper today. The implant is less expensive over a lifetime.
Patient B: 68-year-old who has worn dentures for 12 years. The bone loss from years without implants is significant. A full implant-supported restoration is possible but requires bone grafting and multiple implants. The total cost is substantial. After calculating how many denture relines, adhesives, and replacement dentures have been purchased over 12 years — and valuing the quality-of-life improvement from eliminating the instability, embarrassment, and dietary restrictions of full dentures — many patients in this situation consider the investment justified. Financing through Cherry makes the upfront cost manageable.
Patient C: 35-year-old with an inherited small jaw and two congenitally missing teeth. Waiting is not an option — the spaces are already causing bone loss and tooth migration. Two implants now prevent progressive damage to the entire arch. At 35, this patient will have these implants for 50-plus years if they maintain good care. The per-year cost of the investment is minimal.
How Does Cherry Financing Make Dental Implants Accessible?
The most common reason patients delay implant treatment is upfront cost. Cherry Financing, which Prosper Periodontics offers directly, removes that barrier by allowing patients to start treatment immediately and pay over time. Cherry offers flexible plans, starting from as little as $0 down with monthly payments that fit most household budgets. The application takes minutes and does not require perfect credit.
For a single implant at $4,500 total cost, monthly payments with Cherry start around $100 to $200 per month depending on the plan term and approved rate. For context, that is less than many patients spend monthly on coffee, streaming services, or a car payment. For a treatment expected to last 25-plus years, the math typically favors moving forward rather than delaying.
Delaying implant treatment has a compounding cost that most patients underestimate. Every month without an implant, bone continues to resorb. After 12 to 18 months, a simple implant case may require a bone graft that adds $1,000 to $2,500 to the total cost. The patient who delays a $4,500 procedure often pays $6,000 to $7,000 eighteen months later. Cherry financing makes starting today the financially sensible choice, not just the convenient one.
To learn whether you qualify for Cherry financing and to get an exact treatment estimate, call our office at (972) 787-1122 or request a consultation online. We will review your specific situation and walk through the full cost picture before you make any commitment.
How Do Dental Implants Compare to Other Tooth Replacement Options?
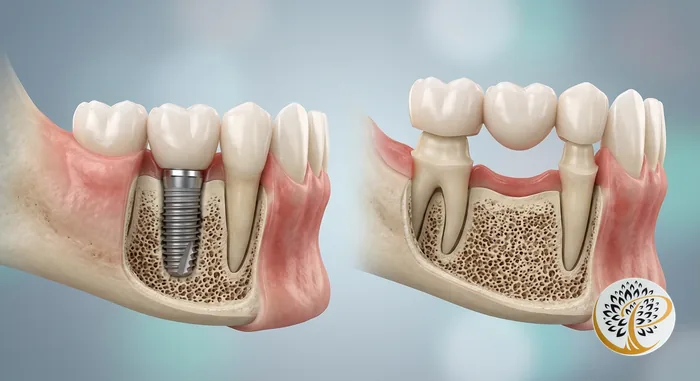
The three main options for replacing a missing tooth are a dental implant, a fixed bridge, and a removable partial or full denture. Each has a different profile of upfront cost, lifespan, functional performance, and biological impact on the surrounding teeth and jawbone.
Fixed bridge: pros and cons. A bridge does not require surgery and delivers a fixed, stable result. Many insurance plans cover a portion of the cost. The significant downsides are that healthy adjacent teeth must be permanently altered (a process called tooth preparation), the area under the bridge is difficult to clean and prone to decay, bridges have a finite lifespan of 7 to 10 years, and bone loss continues beneath the bridge because there is no implant stimulating the jaw. Bridges are a reasonable choice for patients with specific medical contraindications to implant surgery, but they are not equivalent to implants in biological value.
Removable dentures: lowest cost, highest compromise. Dentures are the least expensive upfront option and require no surgery. They are also the option that delivers the worst long-term functional and biological outcomes. Bone loss accelerates dramatically under a denture because the tissue-borne pressure of chewing does not stimulate bone the way a root does. Denture stability decreases as bone continues to resorb, which creates a cycle of refitting and replacement. Full denture patients often find themselves socially restricted by instability, adhesive dependency, and dietary limitations within 5 to 10 years of initial placement.
Dental implants: highest upfront investment, highest long-term value. For patients who are healthy candidates, dental implants deliver the highest functional performance, the best bone preservation, the longest lifespan, and the highest patient-reported quality of life of any tooth replacement option. The clinical consensus among periodontists and prosthodontists is that implants are the standard of care for single-tooth replacement in appropriate candidates. Learn more about your specific options at our dental implants service page or explore All-on-4 full-arch solutions if you are missing most or all of your teeth.
Related Resources
- Dental Implants at Prosper Periodontics – Full procedure overview, candidacy information, and our implant protocol
- All-on-4 Full Arch Implants – Complete-arch restoration in a single procedure
- Specialized Procedures – Bone grafting, sinus lifts, and other preparatory treatments
- Meet Dr. Parachuru – PhD Immunology, specialist training at University of Minnesota
- Dental Implants for Frisco Patients – Serving the Frisco community from our Prosper office
- Dental Implants for Celina Patients – Serving Celina and surrounding areas
- Dental Implants for McKinney Patients – Serving McKinney and north Collin County
Serving Prosper, Frisco, McKinney, Celina, and all of North Collin County. Prosper Periodontics and Dental Implants is located at 2300 E Prosper Trail Suite #20, Prosper, TX 75078. Call (972) 787-1122 to schedule your implant consultation. Monday through Thursday 8am to 5pm, Friday 8am to 12pm.
