How Long Do Dental Implants Last? Lifespan & Maintenance

Dental implants are the longest-lasting tooth replacement option available, with clinical studies reporting 25-year survival rates above 90 percent and many patients keeping their implants for life – making them a true permanent solution when properly maintained. Unlike bridges or dentures that wear out and require replacement, a well-placed, well-maintained implant can outlast every other dental restoration in your mouth. Here is what the science says, what threatens that longevity, and how to protect your investment.
What Does the Research Say About How Long Dental Implants Last?
The most comprehensive long-term studies on dental implants report 10-year survival rates of 95 to 98 percent and 20-year survival rates of 90 to 95 percent, with many implants documented as functional at 30 to 40 years in case reports.
The landmark Branemark studies, which followed the original patients who received titanium implants beginning in the 1960s, documented functional implants at 20 to 30 years post-placement. More recent systematic reviews of modern implant systems with refined surface textures report even higher short-term success rates as surgical and materials technology has improved.
It is important to distinguish between implant survival (the fixture remains in the jaw) and implant success (the fixture functions without complications). The survival rate is higher. An implant can survive in the jaw for decades while its crown requires replacement due to wear, which is a normal and expected maintenance event distinct from implant failure.
Clinical Evidence
Long-term follow-up of osseointegrated implants showed a cumulative survival rate exceeding 91 percent at 15 years when supported by regular maintenance and non-smoking status. — International Journal of Oral and Maxillofacial Implants (Lindquist LW, Carlsson GE, Jemt T, 1996)
What Is Osseointegration and Why Does It Determine Long-Term Success?
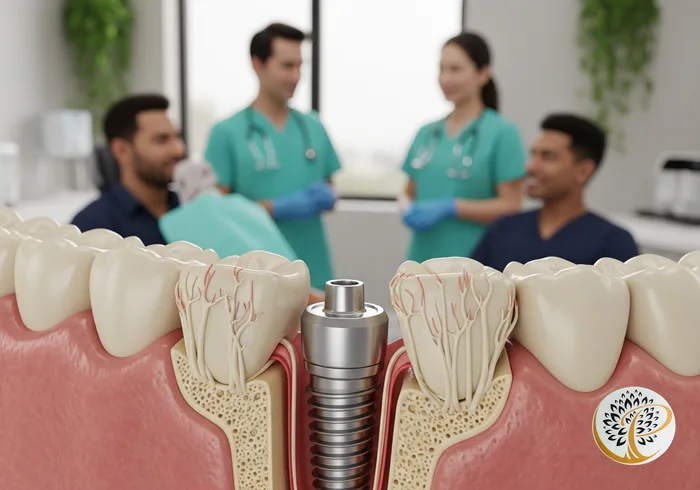
Osseointegration is the direct structural and functional connection between living bone and the surface of a titanium implant – and it is the biological event that makes dental implants permanent.
When a titanium fixture is placed into prepared bone, the surface is not smooth. It is micro-textured through acid etching, sandblasting, or laser treatment to create a rough topology at the micron scale. Bone-forming cells (osteoblasts) attach to this surface and begin depositing new bone matrix directly onto the implant. Over 3 to 6 months, bone weaves into and around the implant surface until the fixture is mechanically locked in place – not with cement or adhesive, but with living bone.
This bond, when fully established, is stronger than the surrounding cancellous bone. The implant cannot be wiggled, pulled out, or dislodged without a surgical procedure. This is fundamentally different from every other dental restoration, which sits on top of tooth structure rather than fusing to it.
Once osseointegration is achieved, the implant fixture typically remains stable for life. The long-term threats to implant longevity are almost never failure of osseointegration after it has been established – they are biological and mechanical events that occur at the implant-gum interface over time.
What Is Peri-Implantitis and Why Is It the Biggest Threat to Implant Longevity?
Peri-implantitis is an infection of the tissue and bone surrounding a dental implant, and it is the leading cause of implant failure – responsible for the majority of late implant losses when it is not caught and treated early.
The condition is analogous to periodontitis (gum disease) around natural teeth. Bacteria accumulate in plaque at the implant-gum junction. If not removed regularly by brushing, flossing, and professional cleanings, the bacteria trigger an immune response that destroys the bone surrounding the implant. As bone is lost, the implant loses its biological foundation and may eventually fail.
A systematic review published in the Journal of Clinical Periodontology estimated peri-implant mucositis (the reversible precursor to peri-implantitis) affects 43 percent of implants, and peri-implantitis affects 22 percent of implants and 10 percent of implant patients over the long term. These numbers sound alarming but they reflect populations with inadequate maintenance. Patients under consistent periodontal care show dramatically lower rates.
Clinical Evidence
Peri-implantitis affects approximately 22 percent of implants at the individual implant level and 10 percent at the patient level in cross-sectional analyses, with higher rates in patients without regular professional maintenance. — Journal of Clinical Periodontology (Derks J, Tomasi C, 2015)
Early Signs of Peri-Implantitis
Because early detection is critical to saving an implant, patients should be aware of these warning signs:
- Bleeding or pus when probing the tissue around the implant
- Redness or swelling of the gum tissue adjacent to the implant
- The implant crown feeling loose or mobile
- Pain or discomfort around the implant during biting
- Visible bone loss on a follow-up X-ray
None of these are normal and all warrant prompt evaluation. If you have an implant and notice any of these, contact our office for an assessment. See our Periodontal Care page to understand how we monitor and treat peri-implant conditions.
What Shortens the Lifespan of a Dental Implant?
Four factors are consistently associated with significantly higher implant failure rates in the clinical literature: smoking, uncontrolled diabetes, poor oral hygiene, and bruxism (teeth grinding).
Smoking
Smoking is the single most modifiable risk factor for implant failure. Nicotine constricts blood vessels and reduces blood flow to healing tissue, impairs immune cell function, and alters the bacterial environment in the mouth. Studies consistently show implant failure rates 2 to 3 times higher in smokers compared to non-smokers. The risk is dose-dependent: heavier smokers have worse outcomes. Patients who quit smoking before implant placement substantially improve their odds. E-cigarettes and vaping present similar risks through nicotine delivery and oral microbiome disruption.
Uncontrolled Diabetes
Diabetes affects wound healing, immune response, and the inflammatory cascade that must resolve normally for osseointegration to occur. Patients with HbA1c above 8.0 percent (poorly controlled diabetes) show significantly higher failure rates and peri-implantitis risk. Patients with well-controlled diabetes (HbA1c below 7.0 percent) have success rates comparable to non-diabetic patients in multiple studies. This is why endocrine control is evaluated before implant placement rather than treating it as a disqualifying condition.
The connection between periodontal disease and systemic conditions like diabetes runs in both directions. Read more in our post on the gum disease, heart disease, and diabetes connection.
Poor Oral Hygiene
Patients who do not maintain adequate home care and skip professional maintenance appointments develop peri-implant mucositis at far higher rates. Left unaddressed, mucositis progresses to peri-implantitis and bone loss. This is largely preventable with the right habits, which is why periodontal maintenance is prescribed as a standing protocol for all implant patients – not an optional add-on.
Bruxism (Teeth Grinding)
Implants integrate with bone but do not have a periodontal ligament, the shock-absorbing fibrous tissue that cushions natural teeth from excessive force. Because of this, implants are less forgiving of excessive bite loads. Severe bruxism creates off-axis forces that can fracture the abutment screw, crack the crown, or – over years – contribute to bone loss around the implant. Custom night guards are strongly recommended for implant patients who grind or clench.
Expert Insight
“The implant itself is almost never the weak link. Titanium doesn't decay, doesn't crack from normal use, and doesn't age the way enamel does. What limits implant longevity is almost always biological: infection at the implant-gum interface or mechanical overload from grinding. Both are addressable when we catch them early.”
— Dr. Parachuru, Periodontist
What Extends the Lifespan of a Dental Implant?
Five evidence-based practices reliably extend implant longevity: rigorous daily hygiene, regular professional maintenance, occlusal protection for grinders, cessation of tobacco, and proactive treatment of peri-implant inflammation when it appears.
Daily Hygiene Protocol for Implant Patients
Brushing twice daily with a soft-bristle brush is the foundation. But implants reward going further:
- Interdental brushes: These fit between the implant crown and adjacent teeth to remove plaque from areas a standard brush cannot reach. They are more effective than floss alone for implant patients.
- Water flosser (oral irrigator): A water flosser delivers a targeted stream that can flush the sulcus (the groove between implant and gum) more effectively than string floss. It is not a replacement for brushing but is a valuable supplement.
- Antibacterial mouth rinse: Chlorhexidine rinse is sometimes prescribed for short periods following implant placement or when early peri-implant mucositis is detected. Long-term daily use is not recommended due to side effects.
Professional Maintenance Schedule
Implant patients should not graduate to a twice-yearly cleaning schedule and consider themselves done. The standard of care for implant maintenance is:
- Every 3 months for the first year post-restoration, to monitor osseointegration and catch early tissue changes
- Every 3 to 6 months long-term, based on your individual periodontal risk profile
- Annual radiographic evaluation to assess bone levels around each implant
At each maintenance visit, the hygienist probes the tissue depth around each implant (just as is done for natural teeth), documents any changes, and uses implant-safe instruments that will not scratch the titanium surface. Our periodontal care team provides this specialized maintenance for all implant patients.
What Happens If a Dental Implant Fails – Can It Be Replaced?
Implant failure does not mean you are permanently without an option – the majority of failed implants can be replaced after appropriate site preparation and healing.
Early failure (within the first few months, before full osseointegration) is typically caused by infection, poor initial bone contact, or a systemic factor that prevented healing. The implant is removed, the site is debrided and often grafted, and re-implantation is performed after healing. Success rates for re-implantation are generally comparable to primary placement when the underlying cause has been addressed.
Late failure due to peri-implantitis requires removal of the implant, thorough debridement of the infected site, bone regeneration procedures if significant bone was lost, and healing before a new implant is considered. This process takes 6 to 12 months but is achievable in most cases.
The decision to re-implant depends on the degree of bone remaining, the patient’s systemic health, and whether the risk factors that led to the original failure can be controlled. This is a nuanced clinical conversation and one Dr. Parachuru approaches on a case-by-case basis.
For a comprehensive overview of the implant process from placement through recovery, see our Dental Implant Recovery Guide.
How Do Implant Crowns and Restorations Age Differently Than the Implant Itself?
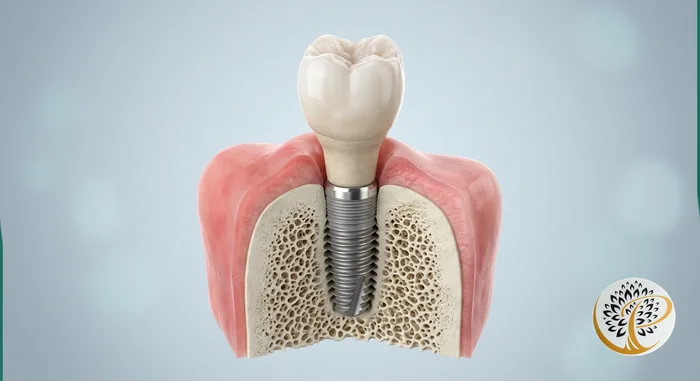
The titanium fixture can last a lifetime, but the visible crown or prosthetic restoration above the gumline has a finite lifespan and will likely need replacement at some point – this is normal and expected, and does not indicate implant failure.
Porcelain and zirconia crowns are highly durable but can chip, crack, or wear over time, particularly in patients with bruxism. Most implant crowns last 15 to 25 years before requiring replacement. The replacement is a straightforward restorative procedure – the new crown is fabricated and attached to the existing abutment without disturbing the implant fixture in the bone.
Full-arch prosthetics like All-on-4 bridges may require more frequent attention. The acrylic or composite teeth in the bridge can wear and chip over 7 to 12 years, prompting a transition to a zirconia prosthetic or repair. This is a planned maintenance event in the All-on-4 lifecycle, not a failure. Learn more at our All-on-4 service page.
Frequently Asked Questions
How long do dental implants last compared to bridges and dentures?
Implants outlast both alternatives significantly. Dental bridges have a median survival of 10 to 15 years before requiring replacement. Full dentures typically require relining every 5 to 7 years and replacement every 10 to 15 years as the jawbone changes shape. Dental implant fixtures, by contrast, are documented lasting 25 to 40 years with maintenance, and many patients keep them for life. See a full comparison in our guide to Single Tooth Implant vs Bridge.
Will I need to replace my dental implant crown?
The crown (visible portion) may need replacement after 15 to 25 years due to normal wear, chipping, or cosmetic changes. This does not mean the implant itself has failed. Crown replacement is a routine restorative procedure that does not disturb the titanium fixture integrated in your jawbone.
Can dental implants fail years after they were placed?
Yes. Late implant failure is most commonly caused by peri-implantitis, which can develop years or even decades after placement if maintenance lapses. This is why regular professional monitoring is a lifetime commitment, not a short-term requirement. Annual X-rays to assess bone levels around the implant are the primary screening tool for late-stage problems.
Does smoking really affect how long an implant lasts?
Substantially. The research consistently shows failure rates 2 to 3 times higher in smokers. Nicotine impairs healing, alters immune response, and promotes the bacterial species associated with peri-implantitis. Quitting before implant placement is one of the highest-value interventions a patient can make to improve their odds. After successful osseointegration, continued smoking still elevates long-term failure risk.
What should I do if my implant feels loose?
Contact your periodontist immediately. A loose implant is not a normal post-operative sensation and indicates either that osseointegration did not occur as expected (early phase) or that significant bone loss has occurred around an existing implant (late phase). Both require prompt clinical evaluation. Do not wait to see if it resolves on its own.
Is there a difference in longevity between upper and lower jaw implants?
Yes, modestly. Lower jaw implants have slightly higher success rates because mandibular bone is typically denser than maxillary (upper jaw) bone, and the upper jaw is anatomically closer to the sinus cavities which can complicate placement. That said, upper jaw implants are routinely successful – the difference in long-term survival rates is small (roughly 2 to 3 percent) and does not change the clinical recommendation.
What happens to my implant if I develop gum disease after it is placed?
Gum disease (periodontitis) and peri-implantitis often coexist and influence each other. Active periodontal disease around natural teeth increases the bacterial load in your mouth and elevates the risk to implants. This is a primary reason why implant patients are kept on periodontal maintenance schedules rather than standard hygiene cleanings. Read more about the treatment of gum disease at our Periodontal Care page and our guide on reversing gum disease.
Schedule Your Consultation
Whether you are considering dental implants for the first time, concerned about an existing implant, or overdue for a periodontal maintenance visit, Dr. Parachuru and the team at Prosper Periodontics and Dental Implants are here to help. Preventive monitoring is the single best investment in implant longevity – and it starts with a conversation. Call us at (972) 787-1122 or book your appointment online.
Related Resources
- Dental Implants – Service Overview
- Periodontal Care and Implant Maintenance
- Dental Implant Recovery Guide
- Dental Implant Cost in Prosper, TX
- Can Gum Disease Be Reversed?
- Gum Disease, Heart Disease, and Diabetes
- All-on-4 Full Arch Implants
Serving Prosper, TX and Surrounding Communities
Prosper Periodontics and Dental Implants provides dental implant placement, periodontal maintenance, and peri-implantitis treatment for patients across Collin and Denton counties. We welcome patients from Frisco, Celina, and the greater McKinney area. Our practice is located at 2300 E Prosper Trail Suite #20, Prosper, TX 75078.
