All-on-4 Implants vs Dentures: Why Patients Are Making the Switch
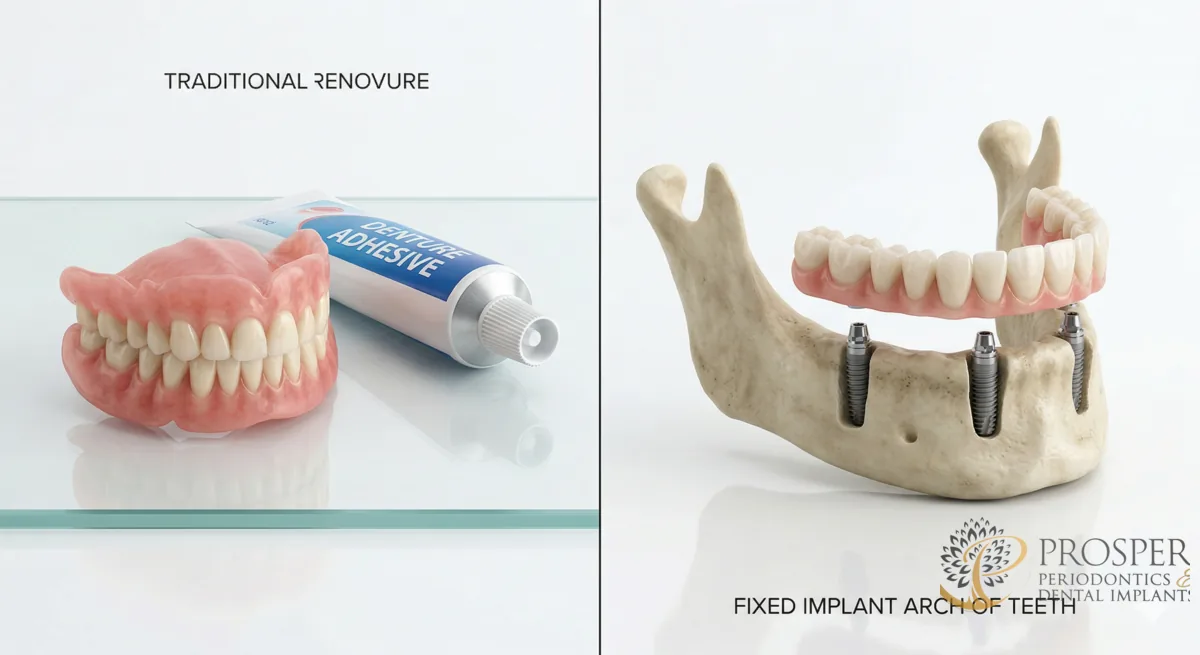
What Is the Difference Between All-on-4 Implants and Traditional Dentures?
All-on-4 implants are permanently fixed to your jawbone and function like natural teeth, while traditional dentures sit on top of the gums and can slip, click, or require adhesive. Both replace a full arch of missing teeth, but they differ dramatically in comfort, function, bone preservation, and long-term cost.
How Do Traditional Dentures Work?
Traditional dentures are removable acrylic prosthetics that rest on the gum ridge. They rely on suction, adhesive paste, or clasps to stay in place. While they restore appearance, many patients struggle with slipping during meals, difficulty eating hard or chewy foods, and progressive bone loss in the jaw that causes the denture fit to worsen over time.
How Do All-on-4 Implants Work?
All-on-4 implants use four strategically placed titanium posts to anchor a full arch of prosthetic teeth directly to the jawbone. The back two implants are angled to maximize bone contact, often eliminating the need for bone grafting. The result is a fixed, permanent set of teeth that look, feel, and function like natural teeth.
All-on-4 vs Dentures: Comparison
| Factor | All-on-4 | Traditional Dentures |
|---|---|---|
| Stability | Fixed — does not move | Can slip and shift |
| Eating Ability | Eat anything — steak, apples, corn | Limited to soft foods for many |
| Bone Health | Preserves and stimulates jawbone | Accelerates bone loss |
| Maintenance | Brush normally, professional cleanings | Remove nightly, soak, adhesive |
| Lifespan | 20+ years (implants are permanent) | 5–8 years before reline/replacement |
| Upfront Cost | Higher ($20K–$30K per arch) | Lower ($1K–$3K per arch) |
Does Insurance Cover All-on-4?
Many dental insurance plans cover portions of the All-on-4 procedure, including extractions and some prosthetic components. Cherry Financing is available for the remainder, making monthly payments manageable.
Ready to ditch the denture adhesive? Schedule a consultation with Dr. Parachuru at Prosper Periodontics. Call (972) 787-1122.
What Happens to Your Jawbone When You Wear Dentures?
This is the biology most denture patients are never told about, and it is one of the most compelling clinical reasons to consider implant-supported restoration. When a natural tooth is lost, the jawbone that surrounded its root loses the mechanical stimulation it relied on to maintain density. Without that daily loading signal, the bone begins to resorb.
In the first year after tooth loss, the bone at the extraction site loses an average of 25 percent of its width and 4 millimeters of height. Over the following years, this resorption continues at a slower but steady rate. After 10 to 20 years of wearing traditional dentures, many patients have lost so much bone volume that the lower jaw takes on a distinctly shrunken appearance and the denture can no longer be supported adequately even with adhesive. This is the “sunken face” look that patients associate with long-term denture wear.
A traditional denture resting on the gum ridge applies pressure to the gum tissue but provides no mechanical load to the underlying bone. Without that loading signal, bone loss continues even while the patient is actively wearing the prosthesis. This is why denture fit deteriorates over time — not because the prosthesis changes, but because the ridge supporting it shrinks.
All-on-4 implants reverse this equation entirely. The titanium posts transmit biting forces directly into the bone through a process called osseointegration, replicating the mechanical stimulus of natural tooth roots. Long-term imaging studies show that implant patients maintain substantially more bone volume than denture-wearing patients over equivalent time periods. The bone does not just stop resorbing — it stays active, dense, and functional for decades.
Clinical Evidence
Long-term studies of edentulous patients demonstrate that conventional denture wearing is associated with continued alveolar bone resorption at measurable annual rates, while implant-supported prostheses preserve bone volume through functional load transmission — Journal of Prosthetic Dentistry (Atwood DA, 2001)
How Does Daily Life Differ Between All-on-4 Patients and Denture Wearers?
The functional differences between All-on-4 implants and traditional dentures become most apparent in the details of everyday life. Patients who make the switch consistently describe changes they did not fully anticipate beforehand.
Eating
Traditional dentures reduce biting force to roughly 25 percent of what natural teeth generate. This forces denture wearers to avoid or carefully modify hard, chewy, and fibrous foods. Steak, raw apples, corn on the cob, hard bread, and many fresh vegetables require avoidance or extensive modification to manage safely. Over years, this dietary restriction contributes to nutritional gaps, as many of the most nutrient-dense whole foods are among the most difficult to eat with dentures.
All-on-4 patients regain approximately 70 to 80 percent of natural biting force once osseointegration is complete and the final prosthesis is placed. Patients eat the foods they want without planning around their teeth. The psychological freedom of that is not a minor detail for people who spent years managing their diet around denture limitations.
Speaking
Traditional dentures can shift during speech, particularly the lower denture, which has less surface area for suction and is perpetually challenged by tongue movements. Many denture wearers learn to speak slightly differently over time — more carefully, less expressively — to minimize the risk of denture movement during conversation. All-on-4 implants do not move. Speech returns to natural patterns within the first few weeks as the patient adjusts to the prosthesis volume.
Social Confidence
The psychological impact of a stable, permanent smile is consistent across All-on-4 patient reports. Denture wearers frequently describe anxiety about public eating situations, concerns about the prosthesis shifting during laughter or animated conversation, and avoidance of social situations centered around food. The fixation of All-on-4 implants removes those concerns. Patients consistently describe a return to spontaneity — laughing freely, eating out without rehearsing the menu in advance, smiling without self-consciousness.
Expert Insight
“The most underreported benefit of All-on-4 implants is what happens to patients psychologically. I have had patients tell me they stopped going to restaurants for years because of denture anxiety. After All-on-4, they describe feeling like themselves again. That is not a cosmetic outcome -- that is a quality-of-life restoration.”
— Dr. Parachuru, Periodontist
How Does the All-on-4 Procedure Work and What Is the Recovery Like?
Understanding the procedural timeline helps patients plan realistically and reduces treatment anxiety. The All-on-4 process typically unfolds across three phases.
Phase 1: Consultation and Planning
3D CBCT imaging maps the entire jaw, identifying available bone volume, nerve positions, sinus boundaries, and optimal implant angulation. A digital treatment plan is created before surgery begins. This pre-surgical planning phase is what makes the all-in-one-day surgery possible.
Phase 2: Surgery Day (Teeth in a Day)
Any remaining teeth are extracted if necessary, all four implants are placed with the back two angled at 30 to 45 degrees to maximize bone contact, and a temporary fixed prosthesis is attached before you leave the office. You arrive without functioning teeth and leave with a complete, fixed smile. Most patients receive IV sedation for this procedure, making the surgical experience comfortable and largely unmemorable.
Phase 3: Osseointegration and Final Prosthesis
Over the next 4 to 6 months, the four implants integrate with the jawbone. The temporary prosthesis allows full function during this period. Once osseointegration is confirmed, the final full-arch restoration — typically milled zirconia for superior strength and esthetics — is fabricated and permanently attached. This is the prosthesis designed to last 15 to 20 years or more.
Recovery from All-on-4 surgery is more involved than single-tooth implant recovery but still dramatically less demanding than patients typically anticipate. Most patients need 3 to 5 days of limited activity. Swelling peaks at days 2 to 3 and resolves by day 7 in most cases. A full liquid and soft-food diet for the first 6 to 8 weeks protects the healing implants while osseointegration begins. For more detail on what to expect during healing, see our complete dental implant recovery guide.
Who Is a Good Candidate for All-on-4 Implants?
All-on-4 is specifically designed for patients facing the loss of all teeth in an arch, those who are already fully edentulous, or patients with so many failing teeth that individual restorations are no longer viable. Candidacy evaluation focuses on three primary factors.
Bone Availability
The angled placement of the back two All-on-4 implants is engineered to bypass areas of bone loss at the molar sites, which are typically the first to resorb after tooth loss. This design allows All-on-4 to succeed in patients who do not have sufficient bone for traditional posterior implant placement, often eliminating the need for extensive bone grafting. However, some minimum bone volume at the implant sites is still required. 3D imaging determines this conclusively during the planning phase.
Periodontal Health
Active periodontal disease must be resolved before implant placement. For patients transitioning from failing natural teeth to All-on-4, Dr. Parachuru creates a comprehensive extraction and implant placement plan that addresses all active infection sites. Treating residual periodontal disease is not a delay — it is what separates a successful long-term outcome from an implant placed into a compromised foundation.
Systemic Health
All-on-4 candidacy follows the same systemic health criteria as single-tooth implants. Well-controlled diabetes, managed cardiovascular conditions, and non-smoking status all support favorable outcomes. Heavy smokers face significantly higher implant failure risk due to impaired tissue vascularity and immune response. Quitting smoking before treatment substantially improves prognosis.
What Is the Long-Term Success Rate for All-on-4 Implants?
All-on-4 implants have over 20 years of clinical outcome data supporting their effectiveness. The original All-on-4 protocol was developed by Portuguese implant surgeon Paulo Malo in the early 2000s, and the peer-reviewed literature since then has consistently documented high success rates across diverse patient populations.
Implant survival rates of 95 to 98 percent at the 5-year mark are consistently reported across major All-on-4 outcome studies. Prosthetic survival rates (the full-arch restoration remaining functional without major complication) are slightly lower over 10-year periods, primarily due to the need for prosthesis maintenance, chipping repairs, or replacement of the removable prosthetic screws — issues that are manageable and predictable.
Clinical Evidence
10-year prospective study of the All-on-4 treatment concept demonstrated implant survival rates of 94.8% in the maxilla and 98.1% in the mandible, with prosthetic survival of 99.2%, supporting the protocol as a predictable full-arch rehabilitation option — Clinical Implant Dentistry and Related Research (Malo P, de Araujo Nobre M, Lopes A, et al., 2011)
These outcomes depend heavily on case selection, surgical technique, and ongoing professional maintenance. At Prosper Periodontics, all All-on-4 cases are planned with 3D imaging, performed with precise implant positioning guided by digital planning, and followed with structured maintenance visits to protect the long-term investment. Patients interested in understanding the full financial picture can review our dental implant cost guide for detailed pricing information.
What Maintenance Does an All-on-4 Prosthesis Require?
The permanent, fixed nature of All-on-4 is one of its strongest selling points, but it does require intentional daily care and professional maintenance to reach its full lifespan potential.
Daily home care involves cleaning beneath the prosthesis bar using a water flosser, implant-specific brushes, or a floss threader to remove biofilm from the implant-gingiva interface. This takes approximately 5 to 10 minutes and becomes routine quickly. Standard brushing of the prosthesis surfaces is also performed twice daily with a soft-bristled brush and non-abrasive toothpaste.
Professional maintenance visits every 6 months include ultrasonic cleaning under the prosthesis, implant probing to assess tissue health, and torque verification of the prosthetic screws — the internal fasteners that hold the prosthesis to the abutments. Screws can loosen over time from normal biting forces and require periodic retightening. At each visit, Dr. Parachuru also assesses bone levels radiographically at appropriate intervals to catch any peri-implant changes before they progress.
Patients who commit to this maintenance protocol consistently achieve the longest prosthesis lifespan and lowest rate of complications. Call (972) 787-1122 or schedule your consultation to discuss whether All-on-4 is the right solution for your situation.
Related Resources
Learn more about the services and topics discussed in this article:
- All-on-4 dental implants
- dental implants
- financing options
- dental implant cost guide
- implant recovery tips
Serving Prosper, TX and Surrounding Communities
Prosper Periodontics and Dental Implants proudly serves patients across North Dallas, including: All-on-4 implants in Frisco, TX, dental implants in Celina, TX. Schedule your appointment today.
