Your First Visit to a Periodontist: What to Expect
What Happens at Your First Periodontal Appointment?
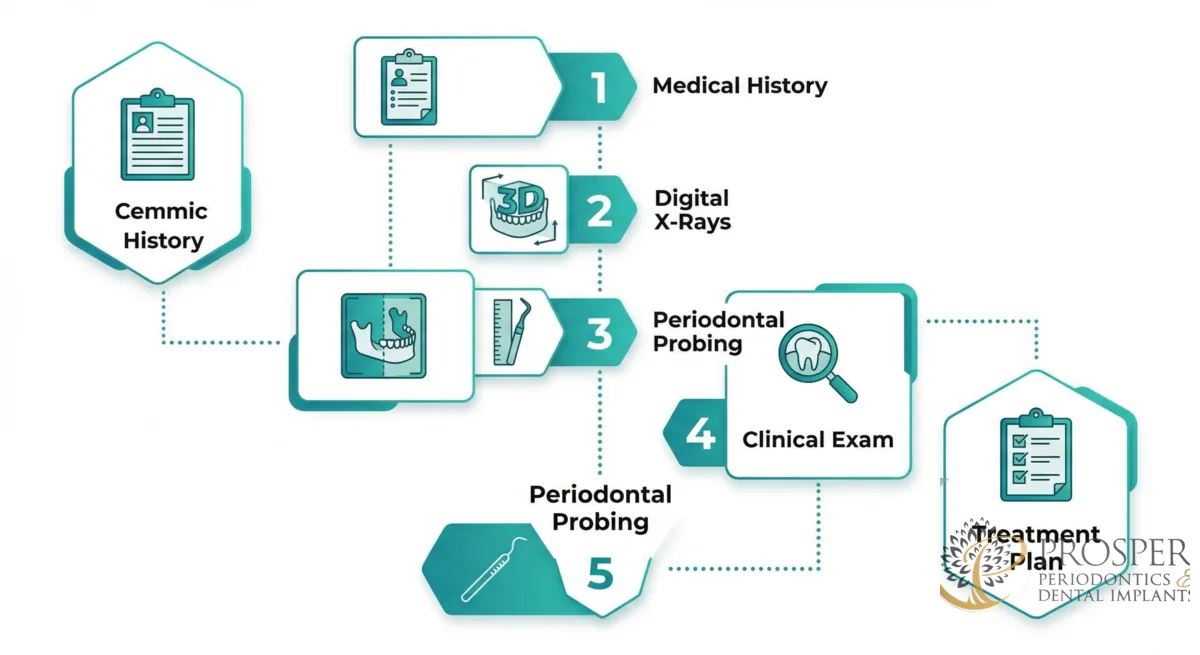
Your first visit to a periodontist typically lasts 60 to 90 minutes and includes a comprehensive examination, digital X-rays, periodontal probing, and a detailed discussion of your diagnosis and treatment options. There is no treatment performed on the first visit — it is entirely diagnostic.
Step 1: Medical and Dental History Review
Your periodontist will review your complete medical history, medications, and any dental concerns. Certain conditions like diabetes, heart disease, and autoimmune disorders can affect gum health and treatment planning. Be open about your full medical history for the safest care.
Step 2: Digital X-Rays and 3D Imaging
We use 3D CBCT imaging to see the full picture of your bone levels, tooth roots, and jaw structure. Traditional 2D X-rays show flat images, but 3D cone beam imaging reveals bone loss, infections, and anatomical details that are invisible on standard films. This technology allows for more accurate diagnosis and treatment planning.
Step 3: Periodontal Probing and Charting
The periodontist will measure the depth of the pockets between your gums and teeth using a small probe. Healthy pockets measure 1 to 3 millimeters. Pockets of 4mm or more indicate gum disease. Pockets of 5mm and above typically require active treatment. Every tooth is charted to create a complete map of your periodontal health.
Step 4: Clinical Examination
Dr. Parachuru examines your gums for recession, inflammation, bleeding, and mobility of teeth. He also checks for signs of oral cancer, bite problems, and any other concerns that affect your treatment plan.
Step 5: Diagnosis and Treatment Plan
You will receive a clear diagnosis and a personalized treatment plan before leaving the office. This includes the recommended procedures, timeline, expected outcomes, and a complete cost breakdown with insurance estimates. There are no surprises — you will understand exactly what is needed and why.
How Should I Prepare for My First Visit?
- Bring your dental insurance card and a photo ID
- List all medications and supplements you take
- Bring any recent dental X-rays if available (your dentist can send them digitally)
- Write down your questions — no question is too small
- If you have dental anxiety, ask about sedation options when scheduling
Ready to take the first step? Schedule your consultation at Prosper Periodontics. Call (972) 787-1122.
What Do the Numbers from Periodontal Probing Actually Mean?
Periodontal probing is the most important clinical measurement your periodontist takes, and understanding what those numbers mean helps you grasp the severity of your situation.
Each tooth is measured at six distinct points: three on the cheek-facing side (buccal) and three on the tongue-facing side (lingual). Those six measurements per tooth are recorded as your periodontal chart — a full-mouth map of your gum health. With 28 adult teeth, a complete charting produces 168 individual measurements.
What the Pocket Depths Mean
- 1 to 3 mm: Healthy. The probe does not penetrate below the gumline significantly. No bone loss present.
- 4 mm: Early inflammation. Bacteria have colonized below the gumline. Bleeding on probing is common at this depth. Treatment depends on full-mouth context.
- 5 mm: Active disease. This is the threshold where most periodontists begin recommending active treatment such as scaling and root planing or laser therapy.
- 6 mm and above: Established periodontitis with measurable bone loss. Deeper pockets harbor more virulent anaerobic bacteria and are significantly harder to maintain with home hygiene alone.
- 7 mm and above: Advanced periodontitis. Tooth mobility, furcation involvement (bacteria reaching the area where roots divide), and significant bone loss are common at this stage.
The chart also records bleeding on probing, furcation involvement grade, tooth mobility (Scale 0 to 3), and gum recession measurements. Together, these data points allow Dr. Parachuru to assign an AAP case classification — Stage I through IV, Grade A through C — which guides treatment planning.
Clinical Evidence
The 2018 AAP/EFP classification system stages periodontitis by severity (I-IV) and grades it by rate of progression and risk modifiers (A-C), providing a standardized framework for diagnosis and treatment planning. — Journal of Clinical Periodontology (Tonetti MS, Greenwell H, Kornman KS, 2018)
What Does 3D Imaging Add That Regular X-Rays Cannot Show?
Standard 2D X-rays show a flat projection of your teeth and bone, which means defects on the front or back of a tooth root are invisible unless they are severe. A 3D cone beam CT (CBCT) scan rotates around your head and reconstructs a three-dimensional image of every millimeter of bone, tooth root, and anatomical structure.
The radiation dose from a dental CBCT scan is 20 to 100 microsieverts (microSv) depending on the field of view — higher than a single periapical X-ray (approximately 5 microSv) but in the same range as a panoramic film (9 to 24 microSv) and well below a medical CT scan of the head (1,000 to 2,000 microSv). The additional diagnostic information routinely justifies this dose for periodontal and implant planning.
For implant planning, CBCT reveals the exact width and height of available bone, the location of the inferior alveolar nerve, and the proximity of sinus floors — all invisible on 2D films. For periodontal diagnosis, CBCT detects angular bone defects, furcation involvement, and root morphology that affects treatment prognosis.
How Will I Know How Serious My Situation Is?
By the end of your first visit, you will have a formal diagnosis using the AAP staging and grading system — not vague language like “you have some bone loss.”
Stage I and II periodontitis indicates limited to moderate bone loss with no tooth mobility. Stage III adds significant bone loss with potential tooth mobility and furcation involvement. Stage IV is characterized by severe bone loss, mobility, and complexity factors that may include masticatory dysfunction.
Grading adds context about how fast your disease is progressing. Grade A is slow progression, Grade B is moderate, and Grade C is rapid progression — often linked to risk factors like smoking or uncontrolled diabetes. A patient with Stage III, Grade C periodontitis needs very different urgency and treatment intensity than Stage II, Grade A.
Expert Insight
“The AAP classification system changed how I communicate prognosis to patients. When I can tell someone they have Stage II Grade B periodontitis, they understand it is serious but treatable, and they understand why we check back every three months rather than once a year. The specificity builds trust.”
— Dr. Parachuru, Periodontist
What Should I Expect Emotionally at My First Visit?
Dental anxiety is real, it is common, and it does not require an explanation or an apology when you arrive. Research consistently shows that fear of judgment is the second-most common barrier to seeking periodontal care, after cost.
Many patients arrive at a first periodontal visit after being told by their general dentist that they “need to see a specialist.” That referral can feel alarming. The common assumption is that a specialist means the situation is severe. That is not always true — general dentists often refer for staging and monitoring, not just advanced treatment.
What you will actually experience at your first visit is a structured information-gathering process. No needles on the first visit. No treatment performed. The goal is to understand your situation completely before recommending anything. Most patients leave feeling relieved — not because everything is fine, but because they finally have a clear picture and a plan.
If you have significant dental anxiety, mention it when scheduling. Our team can arrange for the appointment to be slower-paced, explain each step before it happens, and discuss whether sedation options are appropriate for your future treatment visits.
What Questions Should I Ask at My First Periodontal Visit?
Patients who ask specific questions leave with better outcomes — they understand their treatment, they comply better, and they feel respected in the process. Here are the most important questions to bring:
- “What is my AAP stage and grade?” This gives you a formal, standardized diagnosis rather than a general impression.
- “Is any of this reversible, or is the goal to stop progression?” The answer changes completely depending on whether you have gingivitis or established periodontitis.
- “What happens if I choose not to treat this right now?” Understanding the progression risk makes the urgency concrete.
- “What will my maintenance schedule look like after treatment?” Periodontal maintenance every 3 to 4 months is the long-term commitment — knowing this upfront helps with planning.
- “Does my insurance cover this, and what will my out-of-pocket be?” Ask for written estimates before committing.
- “Am I a candidate for LANAP, or is traditional surgery more appropriate for my case?” Both are valid options; the answer depends on your specific anatomy and disease severity.
What Are the Red Flags During a Periodontal Exam That Signal Serious Disease?
Some findings during a periodontal examination indicate that treatment should begin promptly rather than on a routine schedule. These include:
- Generalized bleeding on probing: Bleeding at 50% or more of probed sites signals active, widespread inflammation across the mouth
- Furcation involvement Grade II or III: This means bacteria have penetrated to where the tooth root divides, creating deep pockets that are extremely difficult to clean
- Tooth mobility Grade 2 or above: A tooth that moves more than 1 mm horizontally has lost substantial bone support
- Pockets of 6 mm or deeper at multiple sites: Deep pockets harbor anaerobic bacteria that produce more destructive virulence factors than bacteria in shallow pockets
- Rapid progression between appointments: If your charting shows significant pocket depth increases compared to records from a prior dentist, Grade C periodontitis (aggressive progression) is possible
None of these findings mean tooth loss is inevitable. They do mean that a wait-and-see approach increases the complexity and cost of eventual treatment. Early action produces better outcomes at every stage.
How Does Insurance Verification Work for a Periodontal Visit?
Insurance verification for periodontal care involves more steps than a routine dental cleaning, and understanding the process in advance prevents billing surprises.
Before your first visit, our team contacts your insurance carrier to confirm active coverage, identify your deductible status, and determine your benefits for specific procedure codes. Periodontal procedures are billed under separate CDT codes from general dentistry. For example, a full-mouth periodontal charting (D0180) is a distinct benefit from a routine prophylaxis (D1110), and not all plans cover it at the same rate.
If your treatment plan includes scaling and root planing, the benefit period timing matters. Most plans cover SRP once per quadrant per 24-month period. If you had SRP recently with your general dentist, your benefit may already be used for that quadrant. Our insurance coordinator identifies these conflicts before treatment begins, not after.
For patients whose treatment plan includes LANAP laser surgery or dental implants, we provide a written pre-authorization submission to your carrier. Pre-authorization does not guarantee payment, but it provides a formal coverage estimate before you commit. Cherry Financing is available to cover remaining balances after insurance.
To learn more about what follows your first visit, read our guide on whether gum disease can be reversed and review the warning signs of gum disease that may have brought you here. If you have been putting off the call, schedule your consultation today at Prosper Periodontics.
Related Resources
Learn more about the services and topics discussed in this article:
- periodontal care
- cutting-edge dental technology
- warning signs of gum disease
- sedation dentistry options
Serving Prosper, TX and Surrounding Communities
Prosper Periodontics and Dental Implants proudly serves patients across North Dallas, including: periodontal care in Frisco, TX. Schedule your appointment today.
