Dental Implant Recovery: Timeline, Tips, and What to Eat
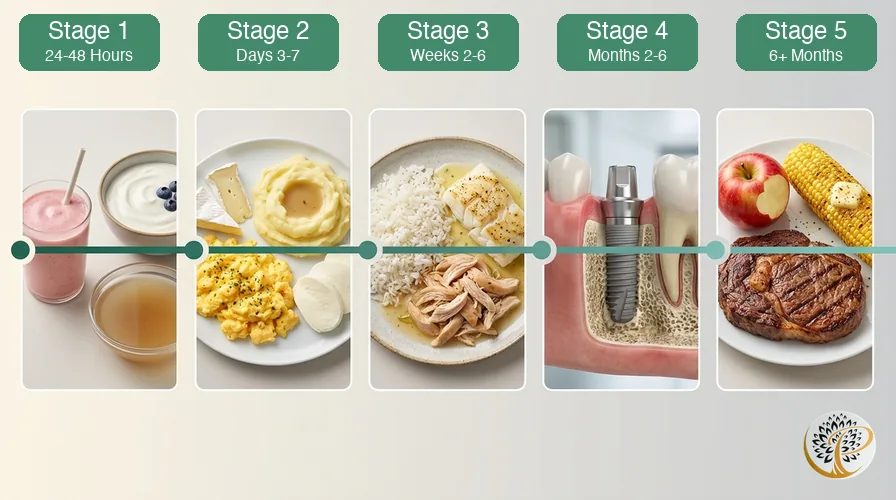
Eating after dental implant surgery progresses through five distinct stages, each with specific dietary guidelines designed to protect the implant, preserve the blood clot, and support osseointegration with the jawbone. This stage-by-stage guide walks you through exactly what to eat, what to avoid, and what to expect at every point in your recovery — from the first 24 hours after first-stage implant surgery through full osseointegration at six months and beyond.
The 5 Stages of Eating After Dental Implants: Quick Reference
Use this table to quickly find the stage that matches where you are in recovery. Detailed guidance for each stage follows below.
| Stage | Timeframe | Texture | Examples |
|---|---|---|---|
| Stage 1 | First 24 to 48 hours | Cool liquids and purees only | Smoothies (no straw), yogurt, cool broth, applesauce |
| Stage 2 | Days 3 to 7 | Soft foods, warm acceptable | Scrambled eggs, mashed potatoes, cottage cheese, soft pasta |
| Stage 3 | Weeks 2 to 6 | Semi-solid, gentle chewing | Well-cooked rice, flaky fish, shredded chicken, soft bread |
| Stage 4 | Months 2 to 6 (osseointegration) | Most foods with caution on implant site | Normal diet minus crunchy foods near the implant |
| Stage 5 | Six months and beyond | Full diet after osseointegration confirmed | Anything — steak, apples, corn on the cob, nuts |
Stage 1: What Can I Eat in the First 24 to 48 Hours After Dental Implant Surgery?
In Stage 1 — the first 24 to 48 hours after implant placement — stick to cool liquids and soft purees only. Heat dilates blood vessels and can re-trigger bleeding at the surgical site. Vigorous chewing or sucking through a straw can dislodge the blood clot protecting the implant. The goal is to stay nourished and hydrated while giving the surgical site complete rest.
Stage 1 safe foods:
- Room-temperature smoothies (sipped from a cup, not a straw)
- Cool yogurt, pudding, and soft-serve ice cream
- Protein shakes and meal-replacement drinks
- Lukewarm (not hot) broth-based soups, spooned
- Applesauce, mashed banana, pureed baby food
Stage 1 strict avoid list: hot foods and drinks, straws of any kind, alcohol, carbonated drinks, seeds, nuts, and anything that requires chewing.
Stage 2: What Should I Eat Days 3 to 7 After Dental Implant Surgery?
Stage 2 covers the first full week after surgery, when the surgical site is sealing and the gum tissue is closing. By day 3, most patients can tolerate warm soft foods that require minimal chewing. Protein intake becomes the priority — target at least 60 grams of protein daily to support tissue repair and bone healing.
Stage 2 safe foods:
- Scrambled eggs and soft omelets
- Mashed potatoes, mashed sweet potato, cauliflower puree
- Cottage cheese and soft ricotta
- Well-cooked oatmeal, cream of wheat, grits
- Soft-cooked pasta with mild sauce
- Flaky baked fish — salmon, cod, tilapia
- Slow-cooked shredded chicken or beef (fork-tender)
Continue to avoid in Stage 2: crunchy foods, sticky candies, spicy dishes, small seeds, and chewing directly on the implant site.
Stage 3: What Can I Eat 2 to 6 Weeks After Dental Implant Surgery?
Stage 3 is the transition phase. Sutures are gone, visible swelling has resolved, and most patients feel recovered — but beneath the gum line, osseointegration is actively happening. You can eat most semi-solid foods, but crunchy and very hard foods remain off-limits to avoid disturbing the implant during bone integration.
Stage 3 safe foods:
- Well-cooked rice and quinoa (once tender, not crunchy)
- Soft breads and muffins without seeds or hard crusts
- Ripe soft fruits — banana, ripe pear, watermelon, peeled peach
- Steamed vegetables cooked through
- Ground beef, turkey, or soft meatballs
- Soft cheeses and dairy
Chew on the opposite side of the mouth from the implant whenever possible. This is the single most protective habit during Stage 3.
Stage 4: What Can I Eat 2 to 6 Months After Dental Implant Surgery?
Stage 4 is the active osseointegration phase. Most of your normal diet returns, but the implant is still fusing with bone at a microscopic level. You will not feel this happening. The golden rule: eat normally, but do not bite directly on the implant site with very hard foods until cleared.
Stage 4 approach:
- Return to most solid foods gradually, testing how each feels
- Avoid biting ice, hard candies, popcorn kernels, or jerky
- Continue to skip very sticky foods that can pull on the site
- Be cautious with small hard seeds (sesame, poppy) that could lodge near the implant
- Attend your follow-up visits — your periodontist confirms osseointegration on X-ray before clearing you for full diet
Stage 5: When Can I Return to a Normal Diet After Dental Implants?
Stage 5 begins once osseointegration is confirmed — typically at the 4 to 6 month mark, and solidly by six months. Your periodontist verifies the implant has fully fused with the jawbone, attaches the final abutment and crown, and you are cleared for a completely normal diet.
At Stage 5, your dental implant functions just like a natural tooth. You can eat steak, crunchy apples, corn on the cob, nuts, and everything else you were missing. The implant is often stronger than the original tooth it replaced, with documented success rates of 95 to 98 percent over 10 years and many implants lasting 25 years or more.
Long-term maintenance for Stage 5 and beyond: clean around the implant the same way you clean natural teeth — brush twice daily, floss or use an interdental brush at the implant site, and maintain 3 to 6 month professional cleanings with your periodontist or dental hygienist. Implants do not get cavities, but they can develop peri-implantitis (an inflammatory condition of the tissue around the implant) if plaque is not controlled.
Learn more in our detailed guide on dental implant costs and value in Prosper, TX, or read about All-on-4 full-arch implants if you are considering multiple implants.
How Long Does Dental Implant Recovery Take?
Initial healing after dental implant surgery takes 1 to 2 weeks, but complete osseointegration — where the implant fuses with the jawbone — takes 3 to 6 months. During this time, the titanium implant becomes a permanent part of your jaw, creating a stable foundation for your crown, bridge, or full-arch prosthesis.
Week 1: The First 7 Days After Surgery
The first week is the most important for healing. Expect mild to moderate swelling, minor bruising, and some discomfort at the implant site. Most patients manage pain effectively with prescribed medication or over-the-counter ibuprofen.
What to eat: Smoothies, yogurt, scrambled eggs, mashed potatoes, soup (lukewarm, not hot), protein shakes, and applesauce.
What to avoid: Hot foods, straws (suction can disrupt healing), alcohol, smoking, and strenuous exercise.
Weeks 2–4: Early Healing Phase
Swelling should be fully resolved by week 2. The gum tissue around the implant is healing and closing over the surgical site. You can gradually introduce softer solid foods like pasta, cooked vegetables, fish, and soft bread.
Months 2–4: Osseointegration Phase
The implant is actively fusing with your jawbone during this critical phase. You will not feel this happening — it is a microscopic process. Avoid biting directly on the implant site with very hard foods. Continue with your normal diet but use common sense.
Months 4–6: Final Restoration
Once osseointegration is confirmed via X-ray, your periodontist will attach the final abutment and crown. At this point, your implant functions exactly like a natural tooth. You can eat anything — steak, apples, corn on the cob.
Tips for Faster Implant Recovery
- Apply ice packs (20 minutes on, 20 off) for the first 48 hours
- Sleep with your head elevated for 2 to 3 nights
- Rinse gently with warm salt water starting 24 hours after surgery
- Do not smoke — smoking dramatically increases implant failure risk
- Take all prescribed antibiotics as directed
- Attend all follow-up appointments
When Should I Call My Periodontist?
Contact Prosper Periodontics immediately if you experience heavy bleeding that will not stop, increasing pain after day 3, fever, or the implant feeling loose. These are rare but require prompt attention.
Planning for dental implants? Call (972) 787-1122 to schedule your consultation with Dr. Parachuru.
What Are the Warning Signs That My Implant Is Failing?
Knowing the difference between normal post-surgical discomfort and a genuine warning sign can protect your investment and your health. Most discomfort after dental implant surgery resolves predictably within the first few days. Pain that worsens after day 3, rather than improving, is the most important red flag to watch for.
Contact Prosper Periodontics immediately if you notice any of the following:
- Heavy bleeding that does not slow down with gentle pressure after 20 minutes
- Fever above 101 degrees Fahrenheit at any point during recovery
- Increasing pain or throbbing after day 3, rather than gradual improvement
- Visible movement or looseness of the implant post
- Persistent numbness or tingling in the lip, chin, or gum beyond 2 weeks
- Swelling that worsens after the first 72 hours instead of resolving
- Pus or foul taste in the area of the implant
Early-stage implant failure is rare, occurring in roughly 2 to 5 percent of cases. When it does happen, it is almost always salvageable if caught quickly. The window for intervention is narrow, which is why prompt communication with your periodontist matters more than waiting to see if symptoms resolve on their own.
What Is Peri-Implantitis and How Do I Prevent It?
Peri-implantitis is an inflammatory condition affecting the soft tissue and bone around a dental implant, and it is the leading cause of late implant failure. Think of it as gum disease for implants. Bacteria colonize the implant surface and the surrounding sulcus, triggering progressive bone loss that can eventually destabilize the implant.
The biology of peri-implantitis mirrors periodontitis in that both are driven by a dysbiotic oral biofilm and an exaggerated host immune response. The key difference is that the implant-tissue interface lacks the periodontal ligament fibers that give natural teeth additional structural defense. This makes implants somewhat more vulnerable once bacterial colonization begins.
Who Is at Higher Risk for Peri-Implantitis?
Certain factors significantly increase a patient’s risk of developing peri-implantitis over time:
- History of periodontitis (the same bacteria can re-colonize implant surfaces)
- Tobacco use (reduces tissue vascularity and impairs immune response)
- Poorly controlled diabetes (elevated HbA1c above 7 is associated with higher failure rates)
- Irregular or skipped professional maintenance appointments
- Inadequate bone volume at the time of implant placement
- Poor oral hygiene after restoration
Clinical Evidence
Peri-implantitis affected 22% of implant patients in a large European cohort, with the strongest risk factors being prior periodontitis history and smoking — Journal of Clinical Periodontology (Derks J, Tomasi C, 2015)
Prevention Starts Before the Implant Is Placed
The best protection against peri-implantitis is a thorough pre-implant evaluation by a trained periodontist. At Prosper Periodontics, Dr. Parachuru uses 3D CBCT imaging to assess bone density and volume, evaluates periodontal health across the entire mouth, and treats any active gum disease before placing implants. This is not a courtesy step. It is a clinical prerequisite that directly affects long-term success rates.
Expert Insight
“I will not place an implant in a mouth with active periodontal disease. Treating gum disease first is not a delay to the patient's treatment — it is the foundation of implant success. An implant placed in an infected environment is an implant that is more likely to fail.”
— Dr. Parachuru, Periodontist
What Is the Long-Term Maintenance Schedule After Dental Implants?
Dental implants are not maintenance-free, and the patients who understand that from day one have dramatically better long-term outcomes. Once your final restoration is placed and osseointegration is confirmed, the focus shifts to a structured maintenance protocol that protects both the implant and the surrounding tissue indefinitely.
Home Care Routine
Daily cleaning around implants requires a slightly different technique than cleaning natural teeth. The implant-crown junction and the gumline are the areas most prone to biofilm accumulation. The following tools and habits form the core of implant home care:
- Soft-bristled electric toothbrush at least twice daily
- Implant-specific interdental brushes or water flossers to clean below the contact area
- Low-abrasive toothpaste (avoid baking soda or charcoal formulas that can scratch implant surfaces)
- Alcohol-free antimicrobial mouth rinse if recommended by your periodontist
Professional Maintenance Visits
Implant patients should return for professional monitoring on a schedule tailored to their individual risk profile. Most patients fall into one of two categories:
- Low-risk (no history of periodontitis, non-smoker, controlled health): Professional cleaning and implant check every 6 months
- Higher-risk (prior periodontitis, smoker, diabetic): Professional maintenance every 3 to 4 months
During each visit, your periodontist will probe around the implant to measure pocket depths, assess bone levels radiographically at appropriate intervals, and check the prosthetic components for wear or loosening. These steps allow problems to be caught at a stage when treatment is straightforward, not after significant bone loss has occurred. Learn more about our ongoing periodontal maintenance and specialized procedures available at Prosper Periodontics.
What Is Osseointegration and Why Does It Matter?
Osseointegration is the direct structural and functional connection between living bone and the surface of a load-bearing implant. The term was coined by Swedish orthopedic researcher Per-Ingvar Branemark in the 1950s after he discovered that titanium could fuse permanently with bone tissue without triggering rejection. That discovery became the biological foundation of modern dental implant science.
The process begins at the cellular level within the first 72 hours after implant placement. Blood clots at the implant site organize into a fibrin scaffold. Osteoblasts (bone-forming cells) migrate into this scaffold and begin depositing new mineral matrix along the titanium surface. By week 4, early-stage woven bone bridges the gap between implant and native bone. By months 3 to 6, this matures into dense lamellar bone capable of bearing full occlusal load.
Modern implant surfaces are engineered to accelerate and optimize osseointegration. Micro-roughened and sandblasted surfaces increase the available contact area, encouraging faster and more extensive bone cell adhesion. This is why implant success rates have climbed over decades of research. Contemporary data consistently shows osseointegration success rates of 95 to 98 percent at the 5-year mark across most patient populations.
Clinical Evidence
Systematic review data supports 5-year implant survival rates of 95.4% for single-tooth implants when placed by trained specialists in appropriately selected patients — International Journal of Oral and Maxillofacial Implants (Pjetursson BE, Tan K, Lang NP, et al., 2004)
What Factors Determine Whether I Am a Good Candidate for Dental Implants?
Not everyone is an automatic candidate for dental implants, but the vast majority of adults who want them can receive them with proper pre-treatment planning. The evaluation performed at your consultation is designed to identify and address any factors that could compromise healing or osseointegration.
Bone Volume and Density
Sufficient bone height and width at the implant site is the most critical anatomical requirement. When a tooth has been missing for a year or more, the surrounding bone typically resorbs inward by 25 to 40 percent. This is why early implant placement after extraction is usually preferable. In cases where bone volume is insufficient, bone grafting can rebuild the necessary architecture before or at the time of implant placement.
Periodontal Health
Active gum disease must be fully treated and stabilized before implant placement. The same bacterial species responsible for periodontitis can colonize implant surfaces and cause peri-implantitis. At Prosper Periodontics, Dr. Parachuru will not place implants until the patient’s periodontal status is fully controlled. This staged approach protects the long-term investment.
Systemic Health Considerations
Most systemic health conditions do not disqualify patients from implants but do require specific pre-treatment management:
- Diabetes: Well-controlled diabetes (HbA1c below 7) is associated with success rates comparable to non-diabetic patients. Poorly controlled diabetes significantly increases failure risk.
- Osteoporosis: Patients on bisphosphonate medications require careful evaluation. A drug holiday may be necessary in some cases.
- Immunosuppression: Managed with appropriate precautions but not an automatic disqualifier.
- Heart conditions: Anticoagulation management and antibiotic prophylaxis protocols are followed as indicated.
Age Considerations
Implants are appropriate for adults once jaw growth is complete, typically around age 18 to 20. There is no upper age limit. Many of the most successful implant patients are in their 60s, 70s, and beyond. Healthy older adults achieve osseointegration rates equivalent to younger populations when their systemic health is well managed.
If you are preparing for implants, the best first step is a consultation with a periodontist who can evaluate your specific anatomy and health history. Call (972) 787-1122 or book online at Prosper Periodontics to get a complete picture of your candidacy and a personalized plan for your dental implant journey.
How Do All-on-4 Implants Compare for Patients Who Need Full-Arch Replacement?
For patients who are missing all or most of their teeth in an arch, the recovery and maintenance principles are the same as for single implants, but the timeline and prosthetic complexity differ. All-on-4 implants use four strategically placed implants to support a full arch of prosthetic teeth, often allowing a temporary prosthesis to be placed on the same day as surgery. Learn more about how this compares to other full-arch options in our detailed All-on-4 vs dentures guide.
What Can I Eat After First-Stage Implant Surgery?
First-stage implant surgery refers to the initial surgical placement of the titanium implant post into your jawbone. Eating requires a soft, cool, non-chewing-intensive diet for the first 24 to 48 hours, with a gradual progression to softer solids through the first week while the surgical site closes and begins healing. The goal is to avoid disturbing the surgical site, the blood clot, and any sutures while your body establishes the foundation for dental implant osseointegration.
What Is the Difference Between First-Stage and Second-Stage Implant Surgery?
First-stage surgery is the implant placement itself — the titanium fixture is surgically seated into the jawbone. Second-stage surgery refers to the uncovering of the implant and placement of the abutment and restoration several months later. In many modern protocols (including same-day and immediate-load cases), these stages are combined into a single visit. If your treatment plan separates them, the dietary rules below apply specifically to the first-stage placement appointment.
First 24 Hours After First-Stage Implant Surgery
Stick to cool, liquid, and soft-puree foods only. Heat and vigorous chewing are the two biggest risks during this window. Avoid anything hot because it dilates blood vessels and can re-trigger bleeding at the surgical site.
- Room-temperature smoothies (no straw — suction can dislodge the blood clot)
- Yogurt, pudding, and ice cream (soft-serve, not bitten)
- Cool protein shakes and meal-replacement drinks
- Lukewarm (not hot) broth-based soups, spooned not slurped
- Applesauce, mashed banana, pureed baby food
Days 2 Through 4: Gradual Soft-Food Progression
By day 2, most patients can tolerate warm (not hot) soft foods that require minimal chewing. The priority is adequate protein intake for healing. Aim for at least 60 grams of protein daily — recovery tissue depends on it.
- Scrambled eggs and soft omelets
- Mashed potatoes, mashed sweet potato, cauliflower puree
- Cottage cheese and soft ricotta
- Well-cooked oatmeal, cream of wheat, grits
- Soft-cooked pasta with mild sauce
- Flaky baked fish (salmon, cod, tilapia)
- Slow-cooked shredded chicken or beef, soft enough to mash with a fork
Days 5 Through 7: Advanced Soft Diet
By the end of the first week, you can typically chew on the opposite side of your mouth from the implant site with soft, forgiving foods. Avoid chewing directly on the surgical site for the full first week regardless of how good you feel.
- Soft bread without crusts or seeds
- Ripe, soft fruits (banana, ripe pear, watermelon)
- Steamed well-cooked vegetables
- Rice and quinoa
- Tender meatloaf, soft meatballs, ground turkey
What Foods Should I Avoid After First-Stage Implant Surgery?
For the full first week after first-stage surgery, avoid anything that can disrupt the blood clot, trap food in the surgical site, or put pressure on the implant before bone integration begins.
- Hot foods and drinks for the first 24 to 48 hours
- Straws for at least 72 hours (suction can dislodge the clot)
- Crunchy foods (chips, popcorn, raw carrots, nuts) for 2 weeks
- Sticky foods (caramel, gummy candy, taffy) for 2 weeks
- Small seeds and grains (sesame, poppy, quinoa when crunchy) that can lodge in the surgical site
- Spicy foods that can irritate healing tissue
- Alcohol for at least 72 hours (interferes with clot formation and any prescribed antibiotics)
- Tobacco for as long as possible — smoking is the single largest modifiable risk factor for implant failure
Can I Drink Coffee After First-Stage Implant Surgery?
Skip coffee for the first 24 hours. After that, room-temperature or lukewarm coffee is fine starting day 2. Avoid piping-hot coffee for the first 3 to 5 days — heat can reopen a healing site and trigger bleeding. If you must have your morning ritual, start with iced coffee or cool brew.
How Much Should I Eat After First-Stage Implant Surgery?
Eat frequent small meals rather than large ones. Prescription pain medication is easier on the stomach with food, and smaller portions are less tiring to chew. Hydration matters more than calorie count in the first 24 hours — aim for 8 to 10 glasses of water or electrolyte drinks. If you had IV sedation, wait until you are fully alert before eating.
Related Resources
Learn more about the services and topics discussed in this article:
Serving Prosper, TX and Surrounding Communities
Prosper Periodontics and Dental Implants proudly serves patients across North Dallas, including: dental implants in Frisco, TX, dental implants in Celina, TX. Schedule your appointment today.
